Nursing Shortage, Identified in 2000, Is Not Yet Eliminated
By Christopher De Los Santos
Photography By Taylor Rice
Reporting Texas

Nursing student Cory O’Connell checks the heartbeat and other vitals of Victoria, the mannequin patient. Taylor Rice/Reporting Texas
It’s no secret that Texas has a shortage of registered nurses. As far back as 2000, the state’s ratio of registered nurses to population was two-thirds the national rate. Eighteen years later, Texas hospital and clinic administrators still can’t hire as many registered nurses as they would like.
From 2000 to 2015, the most recent year for which statistics are available, the number of registered nurses per 100,000 population increased from 612 to 778. In 2017, the national ratio of registered nurses per 100,000 population was 892, according to the Bureau of Labor Statistics and Census Bureau data.
Has the state been the proverbial ostrich, its head in the sand? Not exactly. Texas has studied the nursing workforce, regularly and continuously. The Texas Nursing Association lobbied the Legislature for policy changes to train more nurses. The Legislature acted, but it did so slowly, making a few changes at time, over more than a decade.
Ellen Martin, director of practice for the Texas Nursing Association, calls it legislative foot-dragging. Martin and her TNA colleagues have lobbied the Legislature to act since the turn of the millennium. Martin’s frustration with the Legislature’s slow pace of action rings through clearly in every conversation about the nursing shortage.
State Rep. Donna Howard, D-Austin, says a part-time legislature only solves crises quickly and that substantive reforms take several sessions. Howard holds degrees in nursing and health administration.
The Texas Legislature meets for five months in odd numbered years, unless the governor calls a special session to deal with a crisis. So, as Howard explains, it takes several sessions to identify problems, introduce new ideas, develop solutions and implement new policy. Howard has served in the Legislature for seven sessions and seen this incremental method employed every session for nearly every problem that wasn’t a crisis.
In 2004, the Legislature created the Texas Center for Nursing Workforce Studies to develop an understanding of the nurse shortage and the demographic trends affecting it. It quickly determined that the state had no consensus definition for what constitutes enough nurses.
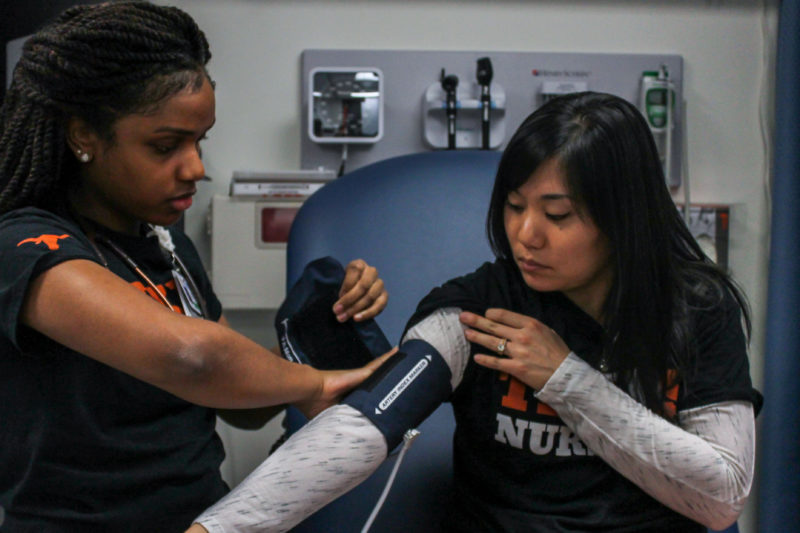
Nursing student Raven Pierre, left, checks the blood pressure of fellow nursing student Emily Hunt, right, during nursing class. Taylor Rice/Reporting Texas
The Department of State Health Services uses the national ratio of registered nurses to 100,000 population as a benchmark. In 2000, according to Census Bureau data and Bureau of Labor Statistics surveys, the national average was 954; in Texas it was 612.
Howard says for the Legislature, the goal is to have a sufficient number of registered nurses (and other health care professionals) to treat the patients moving through the health care system. The Legislature needs a more nuanced understanding of the situation than a simple comparison to the national ratio, Howard says. That’s why it requires the Center for Nursing Workforce Studies to report on a wide variety of demographics and trends within the Texas nursing workforce.
The 2007 legislative session produced several needed reforms. The Legislature revamped requirements for training and education programs that prepare nurses to receive licenses. It also began grants for training partnerships between non-government hospitals and nursing schools. Lastly, the state expanded the use of part-time nursing faculty who work in clinical settings and teach nursing as well.
It wasn’t until 2009 that the Legislature expanded the capacity of nursing schools through grants to existing schools and to startup programs. Licensing standards did not change.
The state began tracking enrollments in nurse training programs in 2008 and published its most recent survey results in 2017. In 2008, 89 programs trained 18,075 nursing students. By 2017, the number of programs had increased to 117 training 23,986 nursing students.
One last problem remained: pay for nursing faculty. Urban hospitals and clinics pay nurses better than colleges and universities or rural hospitals, so the Legislature had to find an incentive to attract more teachers.
In 2011, Sen. Juan Hinojosa, D-McAllen, proposed a bill to fund repayment of student loans for nursing faculty. Every dollar of repaid student debt is worth about $1.30 of income. In 2013, the Legislature authorized up to $7,000 in debt repayment assistance per year for each nursing faculty member — equivalent to a $9,000 pay raise.
By 2016, the reforms had created a new problem. Increased enrollment had overwhelmed available slots for clinical training, where students work directly on patient care under the supervision of a licensed nurse.
“We have not been able to add [nursing students] due to lack of clinical placements,” says Alexa Stuifbergen, dean of the School of Nursing at the University of Texas at Austin.

Nursing students Ryan Webb, left, and Jennifer Schmitz, right, read patient charts in class. Taylor Rice/Reporting Texas
This time, the answer was innovation. Responding to improvements in clinical simulation techniques and technology, The National Council of Boards of Nursing gave simulations its approval in 2003. The Texas Center for Nursing Workforce Studies has tracked clinical simulation as a portion of nurse training since 2010.
“Clinical simulation can go a long way in helping to ease the strain of clinical placements,” says William Scott, associate dean of nursing at Texas Tech. Use of high fidelity clinical simulation training in curriculum increased substantially along with the number of registered nurse training programs in 2013.
The simulations give nursing students rigorous scenarios using advanced training mannequins, Scott says. The mannequins have moved far beyond the life-sized dolls used to train first responders in rescue breathing decades ago. They can exhibit a variety of symptoms and register a variety of treatments and procedures.
Thus, clinical simulations can challenge the students on a fixed schedule, rather than leaving the training up to whatever happens on the ward, says Joanne Spetz, professor at the Philip R. Lee Institute for Health Policy Studies in San Francisco. If a hospital or clinic has a slow day when students are there for training, then students have a slow day as well. With clinical simulations, faculty and students can make the most of every training hour.
By 2018, the shortage of nurses was most apparent in rural counties and along the border with Mexico, according to Martin. Urban counties tend to have a good balance of types of nurses and sufficient numbers to treat patients but many rural critical access hospitals have difficultly retaining registered nurses, even thought they offer substantial signing bonuses
In October 2016, Texas Center for Nursing Workforce Studies published its most recent supply and demand projections. Assumptions in the projections include more Texans getting health care coverage, more Texans living longer, anticipated retirement of current nurses and current nurse training trends.
The gap between nurse supply and demand remains under 10 percent until 2022, when it begins to widen. By 2030, the center foresees a 20 percent shortage; half to two-thirds of that can be made up by available nurses working a reasonable amount of overtime.
Martin says that by 2017, the Legislature had implemented all the policy proposals by the Texas Nursing Association. As of the 2017 Bureau of Labor Statistics figures, Texas had closed its gap with the national average from 22 percent in 2000 to a 12 percent.
Martin, Scott and Gayle Timmerman, associate dean of nursing at UT-Austin, all agree that to continue its improvement, Texas needs to again increase the number, capacity and faculty of training programs. All the tools that worked before will work again when the Legislature makes the issue a priority, they say.