Cadavers Remain Vital Partners in Training Doctors at Dell Medical
By Danielle Smith
Reporting Texas
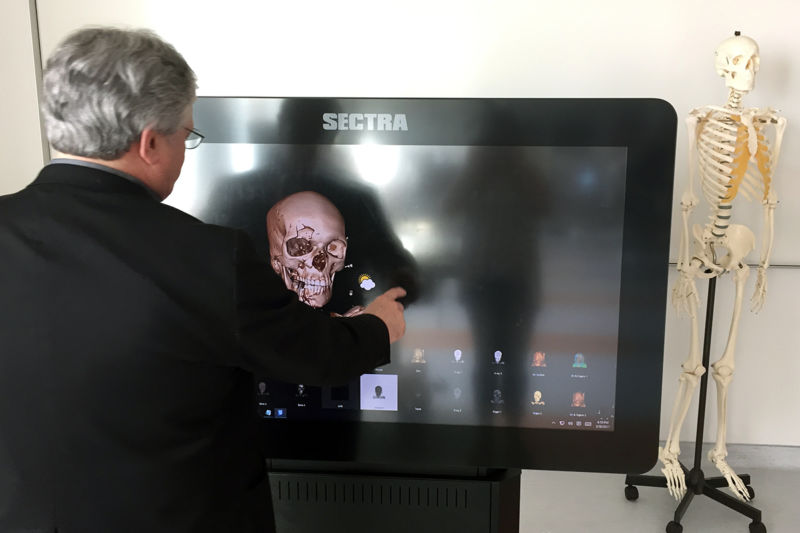
Dr. Brian Miller, head of anatomy at Dell Medical School, works with a touch-screen program that lets students produce three-dimensional renderings of the cadavers they study. Danielle Smith / Reporting Texas
But for its view of the Texas State Capitol, the fourth-floor anatomy lab at Dell Medical School, with its sleek steel gurneys, touch-screen computer monitors and high-intensity lamps, might be mistaken for a futuristic movie set.
Yet it’s here, in this $1 million state-of-the-art facility of the University of Texas at Austin, that students establish one of their most significant relationships in their medical education—the bond between proto-physician and cadaver.
“They’re the selfless silent teachers of the medical school,” said Ariane Lemieux, 24, one of 50 students in Dell Medical’s inaugural class, which began last July. With Dell’s first cohort of students came its inaugural class of six cadavers.
“Things that I saw on my cadaver resonate with me a lot better,” said Lemieux of the eight months of anatomy training each student undergoes. “It was more real than just [relying on] a book.”
Lemieux recalls the time a professor showed her a scar on the shoulder muscle of a cadaver, a possible sign of cancer. Actually seeing scar tissue and learning that it is more susceptible to disease proved an indelible lesson.
Dell Medical’s goal is to combine such palpable learning experiences with the latest technology. That focus comes at a time of debate within the U.S. medical community in the U.S. about excising cadaver studies in favor of cheaper, more easily managed computer software for studying anatomy.
Each workstation at Dell’s anatomy lab is equipped with high-speed internet access and software that lets students and teachers access scans and databases, as they dissect cadavers between June and February, when anatomy is taught.
Dr. Brian Miller, 65, who has taught anatomy for 35 years, accepted the position as the head of anatomy instruction at Dell Medical School last year. “The fact that we have access to [advanced technology] is a fairly significant leap forward in the ability to provide our students with the best educational tools,” said Miller.
Yet technology alone won’t make the grade, as Miller sees it. “Holding a heart in your hand, taking it apart, has sort of a synesthetic quality where all your senses combine to make it a … riveting experience. And that sort of experience isn’t reproduced by any computer program,” he said.
Like medical students, cadavers must meet rigorous qualifications. All organs must be intact—the cadaver can’t have been autopsied or have a record of infectious diseases that might affect major organs.
The practice of human dissection for medical purposes was first recorded in Greece in the third century B.C.E. In Europe, the Catholic Church banned the practice until the 16th century. In the 19th century, as the number of medical schools in the U.S. grew, cadavers were scarce. Grave-robbing and illegal trading in corpses became common among professional thieves, called “night doctors,” who stole buried bodies for medical students. In 1883 Pennsylvania passed the Anatomy Act, which regulated the way licensed institutions acquired their bodies. Other states followed.
Today, willed body programs, in which people bequeath their bodies to medical science, supply the bulk of cadavers used in U.S. schools The programs are governed at the state level and often run by universities.
In Texas, the state Anatomical Board oversees 11 such programs. UT-Southwestern in Dallas operates the biggest willed-body program, and the second-largest in the nation. The university expects to receive over 1,500 cadavers in 2017 from among a list of more than 40,000 prospective donors.
UT-Southwestern supplies cadavers for Dell Medical School and 50 other universities in Texas and beyond. Each cadaver costs about $1,500, but since state law prohibits the sale of bodies, the price tag covers transportation and management costs.
Donors can request that their bodies be gifted to a specific medical school, says Claudia Yellet, a licensed mortician who manages the UT-Southwestern program—and a number of Longhorn alumni have expressed interest in returning after death to help train doctors at Dell Medical.
“We agree to honor a family’s request to go back to Dell if at all possible,” Yellet said in an email. “However, we do make the families aware that currently Dell’s needs are small. As Dell’s needs grow, we hope to ensure that more donors wanting to go back to them are allowed to do so.”
Miller said surveys of prospective medical students show the vast majority would not consider a medical school without cadavers in its anatomy lab.
“A number of computer programs that teach anatomy tend to show an idealized version of anatomy and sort of the average, when in fact, very often it’s anatomical variation that can be important in one way or another to medical professionals,” said Miller.
Bodies arrive at the Dell anatomy lab in June and complete their work in February, after which they’re shipped back to UT-Southwestern to be cremated. Remains are returned to next of kin, interred on the UT-Southwestern memorial garden or given a sea burial, depending on the choice of donor or the family.
Students can be more than a little squeamish when they meet their cadavers. Students watch informational videos and learn rules of respect in handling corpses before ever entering the lab.
“It is not at all unusual to see students come in the first day and be nervous and almost a little scared of what they’re about to encounter. They are crossing a threshold, but the vast majority of students quickly get over any kind of trepidation in dealing with dead bodies,” said Miller.
In January, Lemieux and other first-year students organized a memorial service to honor the six bodies they had studied. Donor families provided short biographies, students performed songs and gave speeches, and Lemieux read poetry.
It was an opportunity for closure. “We couldn’t not do it,” she said. “It was a way to say thank you to them for giving us this opportunity to learn so much.”